The human body needs bacteria. We have good and bad bacteria in our bodies. The good bacterium aids in digestion and wards off infectious bacteria that cause illnesses and disease. Approximately, 98 per cent of bacteria are good for us. For example, penicillin is an antibiotic made from fungus to fight infections in our body. However, the small percentage of bacteria is harmful and may interrupt body functions and attack vital organs, causing illness and disease. We need to keep bacteria from entering the body. One of the most comprehensive ways to keep bacteria from entering the body is through our largest organ, the skin.
- The human body needs bacteria.
- The good bacterium aids in digestion and wards off infectious bacteria that cause illnesses and disease.
Bacteria
The human body needs bacteria. We have good and bad bacteria in our bodies. The good bacterium aids in digestion and wards off infectious bacteria that cause illnesses and disease. Approximately, 98 per cent of bacteria are good for us. For example, penicillin is an antibiotic made from fungus to fight infections in our body. However, the small percentage of bacteria is harmful and may interrupt body functions and attack vital organs, causing illness and disease. We need to keep bacteria from entering the body. One of the most comprehensive ways to keep bacteria from entering the body is through our largest organ, the skin.
- The human body needs bacteria.
- The good bacterium aids in digestion and wards off infectious bacteria that cause illnesses and disease.
Bacteria Invading the Skin
The skin protects the body's internal and external environment against infectious bacteria. The skin works as a protective barrier for invading bacteria. If a bacterium invades the skin, the response system works to remove the bacteria before it is able to enter the body. For instance, if a splinter punctures your skin, the body releases histamine, causing your capillaries to leak white blood cells, swelling the area, allowing proteins to enter the area. These proteins report this condition to the regulatory system to stimulate phagocytes into the infected area. Phagocytes digest dead cells and eat the invading bacteria. When the proteins have finished eating the bacteria and capillaries repair, swelling subsides.
- The skin protects the body's internal and external environment against infectious bacteria.
- These proteins report this condition to the regulatory system to stimulate phagocytes into the infected area.
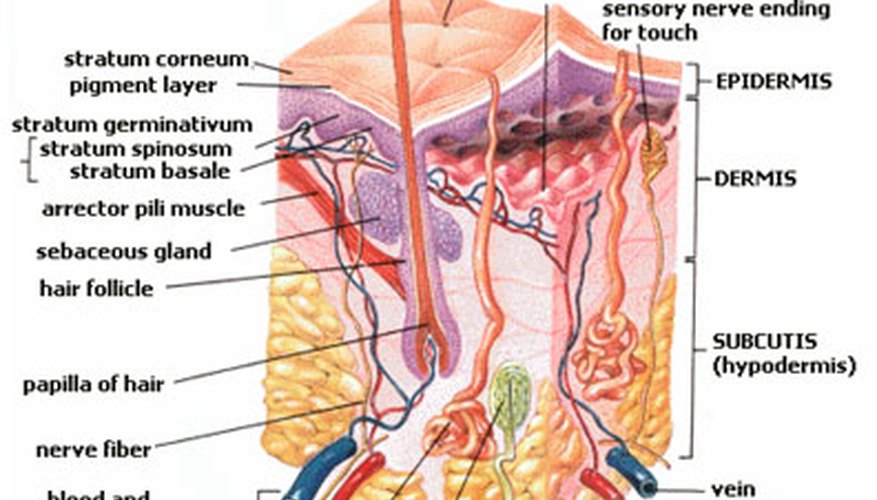
Fighting Bacteria Through the Layers of the Skin
The skin contains seven layers of tissue, and each layer has a function to protect the body from invading bacteria. Some layers produce oil to protect the skin, while others purge toxins through perspiration so the air can evaporate bacteria. The layers also provide skin sensitivities such as tickling and itching to help you brush off threatening bacteria. In addition to preventing bacteria from entering the skin, it can also help the body's internal functions cope with infectious bacteria pending an attack or threatening the body. For instance, when it is cold, our capillaries constrict, inhibiting nutrients and oxygen-rich blood to vital organs. Capillaries are responsible for delivering nutrients and oxygen to the body's vital organs and when the capillaries restrict, the organs do not have a way to ward off infectious bacteria. This is why it is more common to get a cold or flu during the colder months. The hairs on our skin warm our capillaries so they do not constrict. The skin plays an important part in preventing bacteria from entering the body, preventing bacteria from manifesting in the body, and allows healthy bacteria to digest an invading bacterium.
- The skin contains seven layers of tissue, and each layer has a function to protect the body from invading bacteria.
- In addition to preventing bacteria from entering the skin, it can also help the body's internal functions cope with infectious bacteria pending an attack or threatening the body.