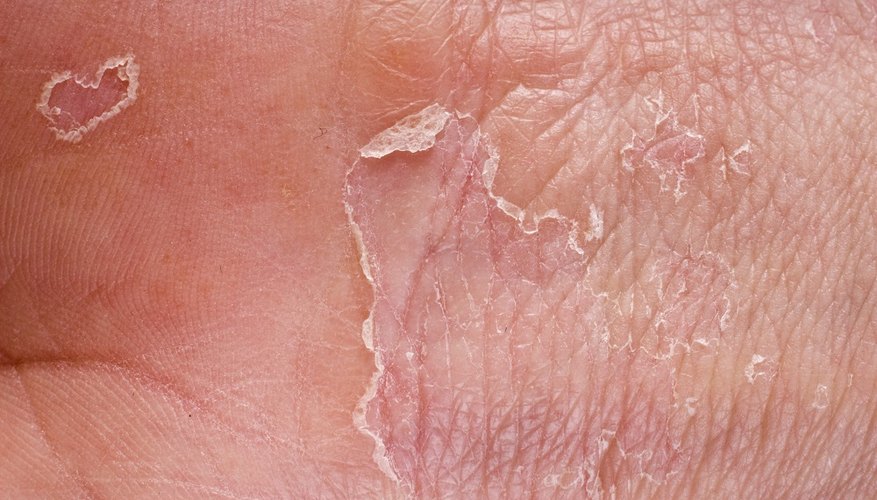
Exfoliative keratolysis is an excessive peeling of the skin on the palm of the hands and is sometimes called "focal palm peeling." The condition is preceded by an outbreak of air-filled blisters across the fingers and palms, which may be caused by eczema. These blisters inevitably burst, causing the palm peeling. In some patients, exfoliative keratolysis is rougher on the tips of the fingers, leaving harder skin that takes longer to heal.
- Exfoliative keratolysis is an excessive peeling of the skin on the palm of the hands and is sometimes called "focal palm peeling."
- The condition is preceded by an outbreak of air-filled blisters across the fingers and palms, which may be caused by eczema.
The peeling of this condition typically does not include itching and can be further irritated by exposure to irritants such as soap and detergents.
Treatment generally includes avoiding exposure to irritants and the usage of hand creams containing some combination of urea, lactid acid and silicone.
In some cases, photochemotherapy, a type of ultraviolet radiation therapy, may be used. Exfoliative keratolysis frequently reoccurs at least once.
Exfoliative keratolysis
Exfoliative keratolysis is an excessive peeling of the skin on the palm of the hands and is sometimes called "focal palm peeling." The condition is preceded by an outbreak of air-filled blisters across the fingers and palms, which may be caused by eczema. These blisters inevitably burst, causing the palm peeling. In some patients, exfoliative keratolysis is rougher on the tips of the fingers, leaving harder skin that takes longer to heal.
- Exfoliative keratolysis is an excessive peeling of the skin on the palm of the hands and is sometimes called "focal palm peeling."
- The condition is preceded by an outbreak of air-filled blisters across the fingers and palms, which may be caused by eczema.
The peeling of this condition typically does not include itching and can be further irritated by exposure to irritants such as soap and detergents.
Treatment generally includes avoiding exposure to irritants and the usage of hand creams containing some combination of urea, lactid acid and silicone.
In some cases, photochemotherapy, a type of ultraviolet radiation therapy, may be used. Exfoliative keratolysis frequently reoccurs at least once.
Hand dermatitis
Hand dermatitis, commonly referred to as hand eczema, varies in cause and symptoms. The condition can be brought on by genetic factors, injury, irritants and allergies. Most often, it is caused by working with the hands, making hand dermatitis very frequent in occupations such as health care, cleaning, catering, metalwork and mechanics. Outbreaks can occur on either the back of the hand, the palm or both. Although cases vary from person to person, the condition typically begins as a red, itchy rash that escalates to blisters, peeling, swelling and cracking. Secondary bacterial infections are common and result in extreme pain.
- Hand dermatitis, commonly referred to as hand eczema, varies in cause and symptoms.
- The condition can be brought on by genetic factors, injury, irritants and allergies.
Hand dermatitis often spreads to other parts of the body. Treatment for hand dermatitis involves either topical or oral steroids and skin moisturisers. If a secondary bacterial infection is present, antibiotics will be prescribed. Extreme hand dermatitis may necessitate the usage of ultraviolet radiation treatments.
Tinea manuum
Tinea manuum are dermatophyte fungi, also known as ringworm fungi. The degree of inflammation that accompanies the peeling of the skin serves as a clue to what type of dermatophyte that has invaded the body.
Anthropophilic fungi are fungi that have adapted to humans and cause a small and less noticeable rash and peeling, while geophilic fungi are used to living in the soil and zoophilic fungi are used to living in non-human animals. Both cause a much more noticeable and extreme reaction when they are present on the human skin.
Regardless of the type of fungus responsible, tinea manuum causes an outbreak of peeling, dryness and itching on the palm of a hand that will grow over time if not treated. Some types of tinea manuum are also accompanied by blisters that both burn and itch. It typically occurs only on one hand and is spread through direct contact with the fungus, either from another infected human, an infected animal or soil contaminated with the fungus. Like other infections caused by fungi, tinea manuum are treated by either topical or oral anti-fungal medications.
- Tinea manuum are dermatophyte fungi, also known as ringworm fungi.
- Regardless of the type of fungus responsible, tinea manuum causes an outbreak of peeling, dryness and itching on the palm of a hand that will grow over time if not treated.
Psoriasis
Psoriasis is an infection that often causes peeling of the hands, although it can occur on other parts of the body as well.
The main symptom of psoriasis, other than peeling, is the presence of a scaly rash on the skin. Medical science has not pinpointed one direct cause of the disease, though there are a number of contributing causes for psoriasis, including genetic predisposition, obesity, stress, injury, hormones and medications.
- Psoriasis is an infection that often causes peeling of the hands, although it can occur on other parts of the body as well.
- The main symptom of psoriasis, other than peeling, is the presence of a scaly rash on the skin.
Infections such as Candida and malassezia (both types of yeasts) and Streptococcal infections can cause or aggravate an inflammation of psoriasis as well. There is no cure for psoriasis, and patients deal with multiple outbreaks over the course of their lives.
Other causes
Although exfoliative keratolysis, psoriasis, hand dermatitis, tinea manuum and psoriasis are the major causes for peeling of the skin on hands, there are numerous other reasons that can be at fault.
Any type of allergy, rash, fungus, medication or irritations can cause skin peeling in some people. Additionally, sun burns, dry skin and excessive perspiring can cause skin peeling on the hands.