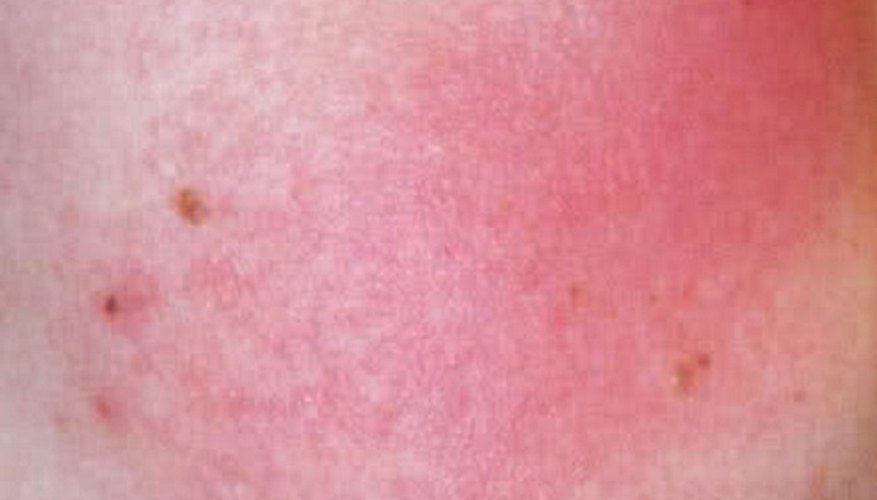
Keratosis pilaris rubra faceii (KPRF) is a skin condition identified by redness and the presence of coarse or rough bumps. Keratosis pilaris rubra faceii can begin at birth or occur during childhood or adolescence. KPRF usually can only be accurately detected and diagnosed on Caucasian patients. Patients with darker skin are often diagnosed with dermatitis.
Symtoms
Symptoms of KPRF include a reddening of the cheeks that is constant and unrelenting. The affected area feels rough to the touch. Doctors can identify the disease by its characteristic crimson colour. KPRF is often misdiagnosed as rosacea.
KPRF is a genetic disorder where the skin begins itching as skin and hair follicles become clogged. In some cases, ingrown hairs will be associated with this condition.
- Symptoms of KPRF include a reddening of the cheeks that is constant and unrelenting.
- In some cases, ingrown hairs will be associated with this condition.
Treatment
Moisturisers and lotions are good for soothing the skin. These treatments may also help reduce skin redness. In some cases, skin creams with urea, lactic acid, glycolic acid, salicylic acid, tretinoin, or vitamin D are prescribed. Treatment of KPRF can often take months. In many cases, symptoms return after treatment is stopped.
In some cases, creams containing vitamin A are good for this condition, ans in other cases doctors may prescribe the acne medication Retin-A. In rare cases, a prescription for the retinoid Adapalene may be written.
- Moisturisers and lotions are good for soothing the skin.
- In some cases, creams containing vitamin A are good for this condition, ans in other cases doctors may prescribe the acne medication Retin-A.
- In rare cases, a prescription for the retinoid Adapalene may be written.
Prognosis
KPRF usually disappears over time. It is most common in young people and disappears naturally as they age. Although the prognosis for this condition is usually very good, it does not respond to over-the-counter medications. As such, it almost always requires treatment by a physician.
- KPRF usually disappears over time.
- As such, it almost always requires treatment by a physician.